LCL Reconstruction
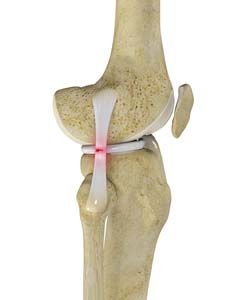
What is a Lateral Collateral Ligament?
The knee is the largest joint of the body and is stabilized by a set of ligaments. In the knee, there are four primary ligaments viz. anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL) and lateral collateral ligament.
The lateral collateral ligament (LCL) is a thin set of tissues present on the outer side of the knee, connecting the thighbone (femur) to the fibula (bone of the lower leg). It provides stability as well as limits the sidewise rotation of the knee.
LCL Injuries
Tears or injury of the LCL may cause instability of the knee that can be either reconstructed or repaired to regain the strength and movement of the knee.
Causes of LCL Injuries
The lateral collateral ligament may tear due to trauma, sports injuries or a direct blow on the knee. A torn LCL may result in pain, swelling and even instability of the knee.
Diagnosis of LCL Injuries
LCL injuries and a torn LCL can be diagnosed through a physical examination and by employing imaging techniques such as X-rays or MRI scan.
Treatment of LCL Injuries
The treatment of a torn LCL may include non-surgical interventions such as rest, ice, elevation, bracing and physical therapy to help reduce swelling and regain activity, as well as strengthen and improve the flexibility of the knee.
Surgery is recommended if non-surgical interventions fail to provide much relief. Surgical interventions include repair and reconstruction of the torn ligament. In case the ligament is torn from the upper or lower ends of attachment, then repair of the LCL is done with sutures or staples. If the ligament is torn in the middle or if the injury is older than 3 weeks, LCL reconstruction is recommended.
LCL Reconstruction Procedure
LCL reconstruction involves the replacement of the torn ligament with a healthy tissue or graft. The tissue or graft can be taken either from a tissue bank (called allograft) or from your own body (called autograft). The type of graft used depends upon your condition and choice of your surgeon. Hamstring tendons are commonly used as autograft, as removal of such tendons does not affect the strength of the legs and effectively stabilizes the knee.
A small incision is made on the lateral side of the knee to perform the LCL reconstruction. The procedure is performed through an open incision and not arthroscopically. The thighbone and fibula are drilled precisely and accurately with specialized instruments to form tunnels. The ends of the tendon graft are passed through tunnels and are fixed by using screws, metal staples or large sutures. The knee is braced for 6-8 weeks.
Postoperative care following LCL Reconstruction
Postoperative you will be instructed to:
- Use crutches to avoid weight bearing on the knee for at least 6 weeks.
- Use ice and prescribed medications to reduce swelling.
- Avoid lifting heavy weights or vigorous exercise.
- Follow rehabilitation programs or physical therapy to regain the motion and strength of the knee.
Risks and Complications of LCL Reconstruction
Some of the possible risks and complications associated with LCL reconstruction include:
- Chronic pain
- Knee weakness
- Knee instability
- Peroneal nerve injury
Related Topics:
- Knee Osteotomy
- High Tibial Osteotomy
- Tibial Tubercle Osteotomy
- Revision Knee Replacement
- Partial Knee Resurfacing
- LCL Reconstruction
- Knee Implants
- Distal Realignment Procedures
- Patellar Tendon Repair
- Cartilage Replacement
- Osteoarthritis Management
- Subchondroplasty
- Meniscal Surgery
- Knee Angular Deformity Correction Surgery
- Unicompartmental Knee Replacement
- OATs (Osteochondral Autologous Transfer Surgery)
- Bicompartmental Knee Resurfacing
- ACL Reconstruction (Patellar & Hamstring Tendon)
- Arthroscopic Debridement – Knee
- Autologous Chondrocyte Implantation
- What’s New in Knee Replacement?
- Minimally Invasive Total Knee Arthroplasty
- Posterior Cruciate Ligament Tear & Reconstruction
- Medial Patellofemoral Ligament Reconstruction
- Cartilage Repair and Transplantation
- Arthroscopic Reconstruction of the Knee for Ligament Injuries